On community nursing, resilience and lifelong learning with Ms Eileen Lau
Find out more about what makes nursing so fulfilling, what a day in the life a community nurse looks like, and why support in the workplace is so important.

This article is part of the Public Health People series where I meet with different public health professionals from all around the globe. Join me in exploring the greatest insights from their fields, their passion projects and their principles for both work and life.
Bound by paperwork, short on hands, sleep, and energy…nurses are rarely short on caring. -Sharon Hudacek
Performing the dual role of clinician and companion, nurses form the largest proportion of the global healthcare workforce. Whether it’s resolving clinical emergencies, soothing patient discomforts or working through tensions within families, nurses are there through and through. In short, nurses are healthcare’s superheroes. As populations around the world age, people are living longer, often with a multiplicity of chronic diseases. Care needs are rising- and so is the demand for nurses. Singapore is no exception.1
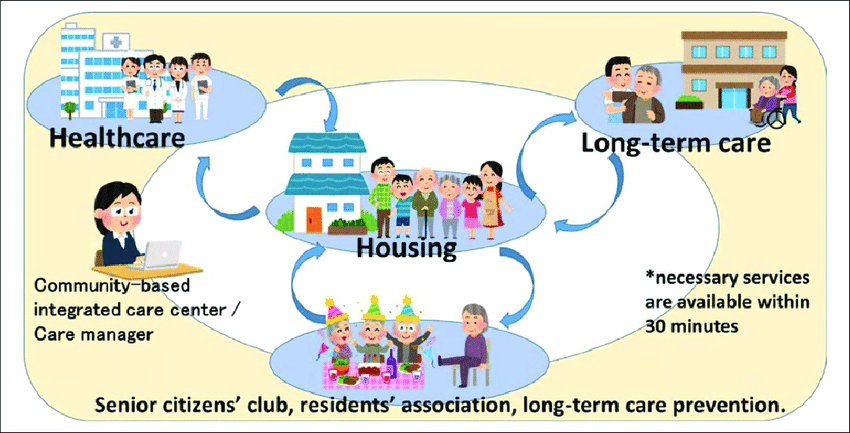
To meet increasing care needs and provide more holistic, patient-centred care, a particular model of care has been gaining momentum across the globe: the integrated model of care. Unlike traditional models of healthcare delivery, integrated care aspires to “place people and their communities at the centre of service provision, rather than their diseases.”2 Integrated care can be summed up in the following diagram:
Today we meet with Eileen, a Senior Staff Nurse at Tan Tock Seng Hospital (TTSH). I decided to meet Eileen, whom I met through a friend because I was curious about what goes on in the daily life of a nurse. She was kind enough to meet with me even after ending work later than usual- she had pulled a 12-hour shift since 7.30 am that day. We warmed up to each other immediately. She spoke with refreshing honesty about the demands of the profession, her unintended path into nursing (hint: she never wanted to be a nurse) and juggling both her job and being a new mother.
I found myself drawn to the easy enthusiasm as she shared her experiences with me. Her passion was in one word, infectious. Underneath her bubbly veneer was also a quiet resilience gained from overcoming the emotional hardships she faced in the early years of her career- something I found admirable and incredibly humbling. In this article, I distil what I learned from Eileen about nursing in the community, how she copes with the demands of her job and insider insights from 10 years as a nurse. I enjoyed this conversation tremendously and I hope you do too.
For students who are interested in Eileen’s journey into nursing: Eileen has a Diploma in Nursing and Advanced Diploma in Nursing (Mental Health) from Nanyang Polytechnic. She has worked at TTSH’s cardiology and psychiatry wards for many years before taking on an exciting new role at the hospital’s Community Health Team. After accumulating over a decade’s worth of clinical expertise, Eileen is currently preparing for her part-time degree programme in nursing to upgrade herself.
NURSES AND THEIR PATIENTS
What does a day in the life of a Community Nurse look like? As a senior staff nurse at TTSH’s Community Health Team (CHT), Eileen’s day starts out with screening through a list of patients that wards, clinics and community partners had referred to the CHT. After rounds of triage, she would focus on the more urgent cases first. “I will call families to ask how they’re coping at home. After assessing their needs, I will assign cases due for their home visits directly to the nurses in the home visit team to see patients,” she says. “After the urgent cases are settled, I will follow up on my existing cases to check on them.” Her day is then followed by meetings with nurses in the wards to decide on the next step of care for current inpatients- Do they have rehab potential? Are ready to be referred to community care services? etc.

On 1-to-1 home visits. Home visits are a chance for both nurses and patients to slow down. Eileen affirms that it’s important to build rapport with her patients. “We don’t jump in immediately to take their blood pressure and other parameters,” she says. “We’ll sit down with the patient and ask them ‘How’s your day?’ or ‘Do you have any problems that you would like to share with me?’” Depending on the patient, nurses might also assess fall risk and the safety of the home environment together with an occupational therapist. Beyond that, Eileen engages in the usual, which includes checking the patient’s parameters; whether patients have been compliant with their medications; and if their caregivers require any clarifications with care. “If there are any issues, we will share how families can provide better care.”
On hospital VS community care. Back in the hospital wards, Eileen was responsible for at least 9 patients at any one time. Now, during her home visits in the community, she is responsible for just one. And since there is time dedicated to each patient during a visit, “You get a lot more time with them,” Eileen says. “I learn more about them and find out how they’re really doing- and I really enjoy that. In the wards, you don’t have that kind of luxury.” This arrangement is also best for patients. Not only can they receive care in the comfort of their own homes, the attention providers can now afford to them helps foster conducive patient-provider relationships.
HOW TO COPE AS A NURSE
When things get rough, use patients to re-centre. Healthcare can be incredibly stressful. Your colleagues matter because they form your primary source of emotional support in the workplace. However, Eileen didn’t have that luxury. “In the first few years, I got picked on a lot. If bosses don’t like you, everybody outcasts you. It got so overwhelming that I used to cry to work every day,” Eileen says. To tide through a difficult work environment, she says that purpose is key. “I find my job incredibly fulfilling. To cope, I went back to why I started and what kept me going,” she says. For Eileen, her drive comes from the patients she serves every day. “They trust me, so I need to do my best for them.”
Put integrity first. What is the single most important thing when dealing with patient lives? Eileen believes it’s integrity. “Patients trust us. You see it when we’re serving medications or administering injections,” she says. As a nurse, you have the responsibility to protect that trust. This means acknowledging when mistakes occur. This means putting aside hardships at work to put patients first. This means following standard operating procedures to prevent slip-ups that can jeopardise patient safety. “Without integrity, you will make mistakes. And when that happens, you put lives in danger,” Eileen says.
Find a mentor. At our lowest points, someone else’s faith in us can be the most uplifting thing. Sister Eng (a nickname) was a nursing officer who entrusted an inexperienced Eileen with opportunities even in her very first year. “She pushed me to grow and even gave me projects to work on,” which Eileen found fulfilling. Because of Sister Eng, her initiatives and performance at work had helped her be recognised with a promotion. “If not for her, I wouldn’t be a nurse anymore. I wouldn’t have pushed myself to go higher.”
Continuously upgrade yourself. The more you know, the more you can help others. Halfway through her career, Eileen took an Advanced Diploma that specialised in nursing for mental health to better serve patients in the psychiatric ward. Her specialised knowledge has been useful in detecting undiagnosed mental illnesses among the elderly during her community rounds. Not willing to stop at just a diploma, she is currently preparing for her part-time degree in nursing. “I need to upgrade myself,” she says. And even though she dreads the stress of juggling work and study, she admits that taking time off to learn specialised skills can serve as a good break too. “As much as I love being a nurse, it’s fun to just focus on studying and hang out with friends,” she says.

Don’t forget what you study in school. If Eileen could go back in time, she’d tell herself to study harder. “I played through my polytechnic years. My GPA was horrible. I didn’t have any goals in my life- I just wanted to complete my diploma,” she says. She learned the hard way that a solid clinical foundation is absolutely necessary. “It was tough when I started work because my knowledge wasn’t fantastic. I couldn’t apply what I learned.” While concepts might seem abstract and far away, what we study in school has a real, tangible application in the field – so pay attention and try to retain the knowledge!
INSIDER INSIGHTS FROM 10 YEARS OF NURSING
On emotional support in the workplace. A great patient experience starts with a great employee experience. How might a hospital best support its nurses? Drawing on her own experience, Eileen believes in creating a safe and empathetic space for all staff. ”The hospital has been very supportive. Now, we have in-house teams you can turn to for counselling,” Eileen says. Building an emotionally supportive workplace also includes respecting time off for recovery and respite. “More than anything, my reporting officers have been wonderful. If I have any stress, I can just talk to them,” she says.

On empowering nurses. There is a world of difference between working in the wards and caring for patients in their homes. Unlike care in the hospital, community care leverages on nurses’ unique clinical expertise and relationships with patients. For one, they are now further empowered to make independent decisions. “I initially had a culture shock,” Eileen says. “I was given the autonomy to make decisions. The patient has a fever. They present other signs and symptoms indicating that they’re unwell. What should I do next?” Their clinical judgements hold more weight now and the added pressure, she says, is welcome. Related: pharmacists and nurses to engage in collaborative prescribing.
On undiagnosed mental illnesses among the elderly. As one ages, social isolation and loneliness become more prevalent worldwide. This puts our elderly at greater risk of conditions such as heart disease and depression. Eileen’s years working in the psychiatry ward has come in handy in her work in the community. “We do see many cases of undiagnosed mental illnesses,” she says. Despite efforts to undo the stigma that cloaks mental illnesses, it is still very much alive across societies. For the elderly, the situation is much more dire. “Oftentimes, they don’t even know that they’re ill, or what mental illnesses are,” Eileen says. Related: Lonely and ‘waiting to die’, Singapore’s elderly poor find hope in many helping hands.
Nursing is hard but fulfilling. One recurring theme among healthcare professionals is that things can get stressful and difficult. Eileen didn’t always want to be a nurse. “Even one small mistake can endanger someone’s life. That’s very stressful,” Eileen says. Yet, once she saw how profoundly rewarding nursing could be during her attachments as a student, she found never looked back. She had found her passion. And this calling to serve those under her care motivates her at work every day. “It’s so fulfilling because you see patients recover under your care. From the moment they’re admitted until they’re back home safely.” Nothing, she says, can compare to that sense of achievement.
In this article, I distilled insights from Eileen about what community nursing is all about, how a nurse might better cope with the stressors of her job and some takeaways from 10 years as a nurse. We explored home visits, how much integrity, passion and lifelong learning matters in nursing, as well as how we are empowering nurses to play a bigger role in healthcare delivery. If you’d like to find out more about nursing as a career, here are some resources you can refer to:
- Resource 1: A guide to nursing career pathways in Singapore.
- Resource 2: Khoo Teck Phuat Hospital’s Community Nurse Home Visit Programme
- Watch 1: You Can Be An Angel- Seasons 1, 2 and 3 by Mediacorp Singapore
Thank you so much for reading!
I would like to thank Anastasiia Sapozhnikova, Gloriana Sojo, Jared Gordon, Rohen Sood, Alysia Harris, Natalie Toren, Riah Forbes, Matt Lerner, Padmini Pyapali for offering their time and generous feedback. I appreciate you guys so much.
- 32 percent of Singaporeans will be aged 65 and above by 2035. https://www.statista.com/topics/5821/ageing-population-of-singapore/ ↩
- Nurjono, M, et al. Implementation of Integrated Care in Singapore: A Complex Adaptive System Perspective. International Journal of Integrated Care, 2018; 18(4): 4, 1–7. DOI: https://doi.org/10.5334/ijic.4174 ↩
Stay updated on the best insights from public health professionals.