The power of moments in patient-centred care

At its very core, patient-centred care is a care approach where the treatment outcome is based on what the patient has defined as meaningful and valuable.I had been thinking about how we can improve our approach to patient-centred care and recalled some examples from a phenomenal book called The Power of Moments by Stanford professor Chip Heath.
At the core of Heath’s groundbreaking book lies the idea that “moments matter”. Heath introduces the idea of ‘defining moments’: short experiences that are both meaningful and memorable. They include things such as falling in love for the first time. Getting fired from your job. Winning a tough competition. Having someone believe in your potential.
Defining moments share four things in common: they are moments of elevation, insight, pride and/or connection. The key takeaway from Heath’s book was all about how we can create more of our own defining moments. He argues,
Defining moments shape our lives, but we don’t have to wait for them to happen. We can be the authors of them. What if a teacher could design a lesson that students were still reflecting on years later? What if a manager knew exactly how to turn an employee’s moment of failure into a moment of growth? What if you had a better sense of how to create lasting memories for your kids? And this led me to think about patient-centred care.
Hence, In this article, I share three examples from Heath’s book about how we can journey towards patient-centred care by creating defining moments of connection and elevation. I’ve outlined three ways, arranged by level of difficulty.
They are:
1. Ask, “What matters to you?
2. Design to elevate.
3. Build strong bridges between employees.
Let’s dive right in.
Level 1: Ask, “What matters to you?”
People in healthcare are problem-solvers. When our patients reach out, we ask, “What’s the matter?” and begin formulating a solution to their problems in our minds. But patients don’t recall how efficient the x-ray machine was, or how fast their painkiller had worked. They remember whether their doctors were good listeners, or if the nurse had asked about their day. They remember whether they felt heard, comfortable and safe.
So, here’s a chance to create a defining moment. Instead of asking your patient, “What’s the matter?”, turn it around and ask “What matters to you?” It’s a simple but profound switch. The children’s wards in all of Stockholm’s hospitals gives us some insight into how powerful this question can be.
Kendra’s Story
Seven year-old Kendra was a new patient at one of Stockholm’s hospitals. On her first day, she had been given some paper and markers to doodle on her “What Matters to Me” page. Kendra has autism and had relied on her father to communicate with the staff because she had never spoken a word before. What happened next could have been a disaster: Kendra’s father had a heart attack and had to be rushed to another hospital to be treated. She was left alone, without anyone to help communicate her needs to the nurses.
Fortunately, Kendra had already completed her drawings on her ‘What Matters to Me page’. On it, she shared the following:
- I have autism. I can’t speak so I won’t be able to if it hurts.
- I don’t like medicine by my mouth so watch out I will struggle.
- I love to feel people’s hair, it is my way of saying hello.”
- I love cuddles to reassure me.

Without Kendra’s “What Matters to Me” page, the staff could have easily misunderstood Kendra as a difficult child that not only refuses oral meds, but also grabs at their hair. But that didn’t happen. The nurses knew to avoid oral medications whenever they could. They cuddled and hugged Kendra. They allowed her to touch and comb through their hair. This question created a moment of connection between the nurses and Kendra. What followed immediately after was understanding, validation and care for Kendra’s needs.
Think about your most precious memories with your patients. How many of these memories were because you shared an intimate connection? What this question does is to set up the stage for connection between patient and care provider. You’re saying, your concerns are important to me. I hear you and I’ll try my best to meet your needs. It’s an opportunity for the patient to feel understood, validated and cared for. Asking “What matters to you?” is easy but profoundly impactful.
As we’ve seen in Kendra’s story, it guides care and resolves misunderstandings upfront. It allows us to see the patient as a whole person, rather than an amalgamation of problems to diagnose and solve.
Level 2: Design to elevate.
Moments of elevation include moments such as birthday parties, weddings, and spontaneous adventures. They usually hold an element of surprise. This is because they break the script of a mundane routine. We can also create moments of elevation in the healthcare setting to deliver memorable experiences for our patients.
How does an MRI machine look like to a child?
Our second story is about Doug Dietz, an industrial engineer from General Electric. He had worked two long years on a new design of an MRI machine back in 2007. He was excited to see his machine being used by patients for the first time. However, when he saw that his first user would be a little girl, he realised he forgot something important.
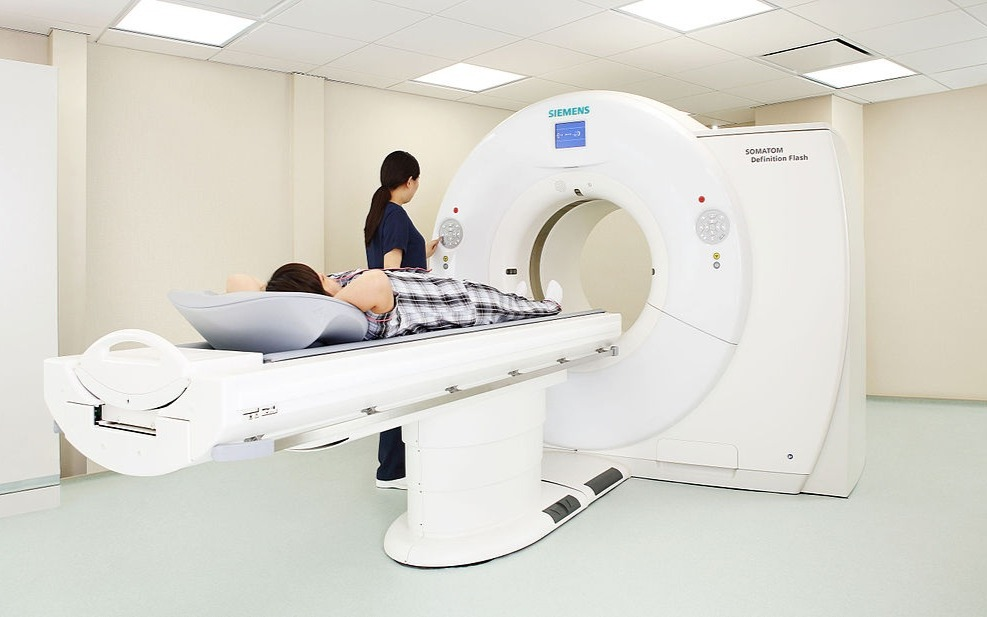
How does an MRI machine look like to a child? Dietz recalls the heartbreaking scene a little girl shrinking in terror at the sight of his creation. In a dim room with flickering lights, all she saw was a gigantic, intimidating apparatus. As part of the scan, she also needed to hold still (sometimes for up to 30 minutes) while surrounded in a space filled with metallic whirrs and unfamiliar sounds. It was going to be a claustrophobic experience.
In fact, children like her were often sedated to help them hold still, but this practice carries health risks. What if Dietz could transform the moment for his patient from a pit to a peak? He decided to engage the help of design thinking experts and healthcare staff who worked with children. And with a few tweaks, his team converted the MRI scan experience into one that leveraged on something powerful: a child’s imagination.
Let’s just take one example from Dietz’s work.
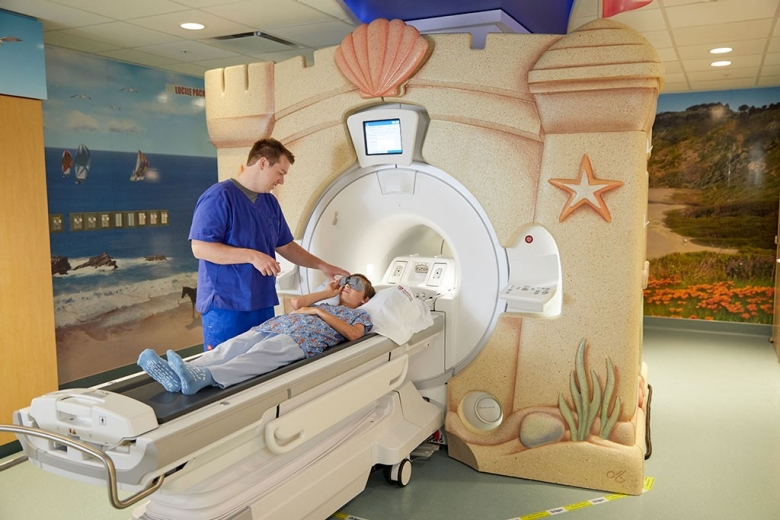
“One of the first rooms they designed, for the University of Pittsburgh Medical Center, was known as the Jungle Adventure. In the hallway leading into the room, the team placed stickers on the floor that looked like rocks. The kids would instinctively hop from one rock to the next. All the walls inside the room were painted in rich, colourful jungle scenes. And the rocks from the hallway led to a painted koi pond, stocked with fish, which surrounded the machine.”

“The MRI table lowered so that children could climb on top. It had been redesigned to look like a hollowed-out canoe, and the kids were urged to hold still so they wouldn’t tip over the canoe as it floated through the jungle. In his talk, Dietz mimed a kid with his arms straight down at his side with only his eyes moving. “These kids are like statues—they’re frozen,” he said.” As a result, the number of children that required sedation to go through the procedure had fallen from 80% to a mere 27%. The scans take place faster, the hospital completes more in a day, and the patient experience is enhanced- a win on all fronts. Some children even asked, “Can we come back tomorrow?” All of this was because Dietz and his team responded to what was valuable to their patients- and beyond. They had transformed what was usually a moment of anxiety and terror into one of adventure and excitement. The experience had been elevated.
Putting the patient experience at the very centre of healthcare is not just rewarding for the patient. Us providers benefit too. Just recall the last time you went above and beyond for someone else (doesn’t have to be patient). It must have triggered a bunch of feel-good emotions for you.
Imagine the possibilities if we could engineer such moments into our existing system. Yes, building peak moments into our system can be difficult and time-consuming at the start. But once these systems become scalable, their rewards compound. A good place Health recommends for us to start would be to identify ‘pits’: anxiety or frustration points in the patient experience. Then, through empathetic design, elevate them to transform them into ‘peaks’.
## Level 3: Build strong bridges between employees.
In the first two sections, we’ve explored two paths towards patient-centred care. First, asking, “What matters to you?” (Level 1) and second, designing moments of elevation (Level 2). Now, let’s look at reaping the benefits of Levels 1 and 2 in a sustainable way. Here, we look to Level 3, arguably the most difficult, but most rewarding step of all.
As the book mentions, we can’t create a great patient experience without a great employee experience. And one important way of creating a great employee experience is to build strong ties between employees. There is one tried and tested way of doing so. That is to have people engage in a common struggle towards a shared, meaningful end.
“For groups, defining moments arise when we create shared meaning—highlighting the mission that binds us together and supersedes our differences. We are made to feel united.”
Recall a time when you and your colleagues struggled together to solve a difficult problem. It could be a task to alleviate a patient’s persistent pain; a task to devise a complex care strategy for a patient’s unique socio-economic background- anything, so long as it was a joint struggle with a meaningful outcome. I bet you came out feeling a stronger sense of solidarity with one another.
Well, within joint, meaningful struggles lies an opportunity to create defining moments of elevation and connection. The magic of bringing 12,000 staff together. Our third story is about Sharp HealthCare, a regional healthcare group based in San Diego. In 2001, they had a new vision to transform the health care experience and make Sharp:
- The best place for employees to work
- The best place for physicians to practice
- The best place for patients to receive care
- Ultimately, the best health care system in the universe.
Their vision was bold. In order to have the entire corporation take their new vision seriously, the executive team at Sharp decided to create a defining moment. And that is to have all 12,000 of their staff meet one another. What initially sounded like a ludicrous idea ended up revolutionising both Sharp and patient care. This idea eventually came to life as the annual All-Staff Assembly, a gathering of all 12,000 healthcare staff members from Sharp Healthcare divided across three days.
Just imagine being surrounded by 4000 strangers at a high-energy event where individuals and groups were celebrated; speakers were brought in to inspire; everyone was invited to brainstorm ways they can “create magic for those you serve”.

It was a peak moment, a moment of elevation: the script had been broken! None of Sharp’s staff had ever attended a gathering of such an extraordinary scale, nor have they met so many others from the same team before.
What the assembly did was to create a profound sense of solidarity among the staff: that we’re all in this together and what we’re doing matters. It was a moment of deep social connection. And the glue that bound the staff together was a renewed sense of purpose. The executive team went one step further. At the Al-Staff assembly, the employees at Sharp were invited to volunteer to improve the patient experience in order to achieve their new vision.
Why? The Heath brothers share some insights about leveraging the power of purpose in bringing people together:
Passion is individualistic. It can energize us but also isolate us, because my passion isn’t yours. By contrast, purpose is something people can share. It can knit groups together. Once this profound sense of connection is established upstream, the benefits on patient care will spillover. And with the 1,600 people who had volunteered with Sharp came massive leaps forward in patient care and employee satisfaction.
Patients without visitors or flowers received them from the landscaping team. Caregivers were trained to introduce themselves when they greet patients. Upon discharge, patients received handwritten cards from their caregivers and a loaf of banana bread, “baked with love”.
Five years after the first All-Staff Assembly (it has since become an annual tradition), Sharp saw patient satisfaction skyrocket from the tens to the nineties. Physician satisfaction also rose to the 80th percentile in the national percentile rankings; overall employee satisfaction had increased 13% and net revenue had grown by half a billion dollars.
It can be easy to lose sight of why we do what we do as providers of care amidst the daily tedium of work. When that happens, it may become difficult to truly meet the needs of those we are caring for. But there is a solution. By creating moments of elevation and connection, we can re-invigorate teams with a shared sense of purpose.
Celebrate achievements. Ask employees what matters to them. Invite people to brainstorm ways to create magic for those they serve. Create opportunities for joint struggles towards common, meaningful goals.
While there is no need to create an All-Staff Assembly like Sharp, we can definitely identify opportunities to create transformative moments of connection and elevation.
Conclusion
Heath mentioned that people will always try to stop you from creating peak moments. Indeed, they may not be easy to create. But there is one thing about human nature that we can’t deny: that we live our lives in moments. An experience at the hospital can be a life-defining moment. The experience for a patient in the hospital can often be beset with anxiety, sometimes even a crippling fear. But as providers of care, we have the power to turn those pits into peaks.
In this article, we’ve outlined three ways you can start creating defining moments: 1. Ask, “What matters to you? 2. Design to elevate. 3. Build strong bridges between employees. These three methods can be applied to create better experiences for all members of the healthcare ecosystem: research teams, hospital administration, front-line care providers and policy-makers.
When we are driven by purpose, we flourish. When we flourish, our patients flourish too. How might you start creating defining moments for your patients and your team?
Stay updated on the best insights from public health professionals.